So, what’s really behind gum disease? The short answer is plaque—that sticky, nearly invisible film of bacteria that’s always trying to set up camp on your teeth. When you don't show it the door, it starts to irritate your gums, triggering an inflammatory response that is the first step toward gum disease.
The Hidden Culprit Behind Gum Disease
Think of your mouth as a tiny, bustling ecosystem. For everything to run smoothly, it needs balance. The main troublemaker that throws this balance off is dental plaque. This slimy layer of bacteria loves to feast on the sugars left over from your food and drinks. As it does, it releases acids that not only attack your tooth enamel but also seriously annoy your gums.
This isn't a rare problem, either. It’s a massive global issue. It's estimated that nearly 3.5 billion people are dealing with some form of oral disease. More specifically, significant gum disease affects about 45% of adults over the age of 30. You can dig deeper into these global oral health statistics and see just how widespread this is.
This image breaks down the key players that pave the way for gum disease to take hold.
As you can see, while bacteria-filled plaque is the root of the problem, things like poor oral hygiene and certain lifestyle choices create the perfect storm for it to thrive. It’s an issue with many layers, but it all starts with that simple bacterial buildup.
To give you a clearer picture, here’s a quick summary of the factors that work together to cause gum disease.
Key Factors Causing Gum Disease at a Glance
| Factor Category | Specific Cause | How It Contributes |
|---|---|---|
| Bacterial Buildup | Dental Plaque | This primary cause is a sticky biofilm that produces acids and toxins, directly irritating the gums and triggering inflammation. |
| Poor Oral Hygiene | Inadequate Brushing/Flossing | Failing to remove plaque daily allows it to harden into tartar, which can only be removed by a professional and provides more surface area for new plaque. |
| Lifestyle Choices | Smoking & Tobacco Use | This significantly weakens the body's immune response, making it harder for gums to heal and easier for infections to progress. |
| Genetic Predisposition | Family History | Some individuals are genetically more susceptible to developing gum disease, regardless of their hygiene habits. |
| Systemic Health | Diabetes, Hormonal Changes | Conditions like diabetes impair the body's ability to fight infection, while hormonal shifts (e.g., pregnancy) can increase gum sensitivity. |
Understanding these connections is the first step in building a strong defense against gum disease.
The Two Stages of Gum Disease
It's important to know that "gum disease" isn't just one thing; it's a progressive condition. It moves through two main stages, and knowing the difference is key to understanding why it can get so much worse.
- Gingivitis: This is the early, mild, and—most importantly—completely reversible stage. Think of it as your body's first warning signal that plaque has overstayed its welcome. At this point, the infection is only in the gums, leading to symptoms like redness, swelling, and a bit of bleeding when you brush.
- Periodontitis: If gingivitis is left unchecked, it can escalate to periodontitis. This is a much more serious condition. Here, the infection dives below the gumline, actively destroying the tissues and bone that hold your teeth in place. This damage is permanent and, if not professionally managed, can ultimately lead to tooth loss.
The journey from healthy gums to periodontitis starts with one thing: uncontrolled plaque. Recognizing the initial signs of gingivitis and taking action is the most effective way to prevent irreversible damage.
Recognizing Gingivitis: The First Warning Sign
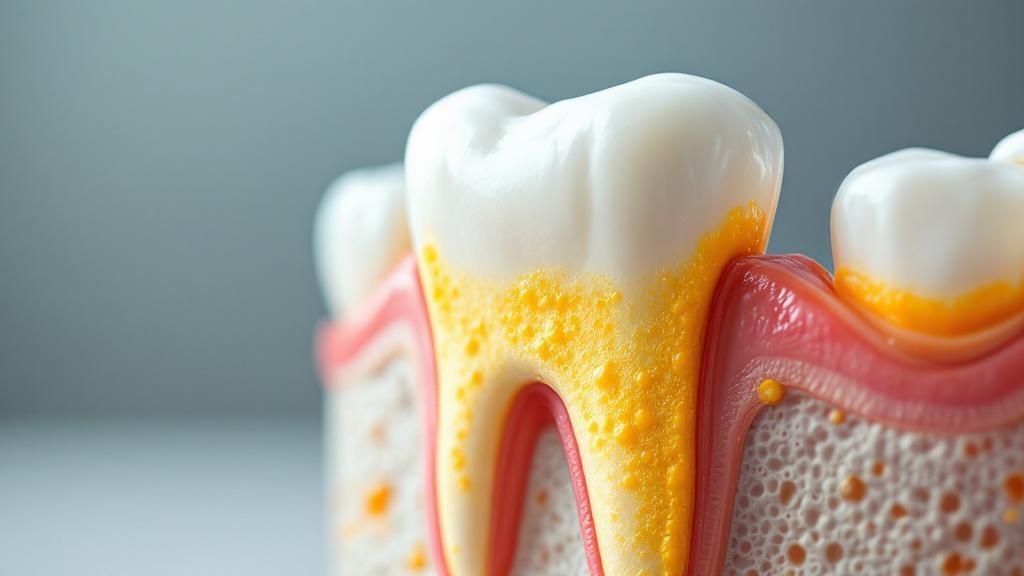
When plaque starts to creep along your gumline, your body doesn't stay silent. It sends out its first alarm bell. This initial stage of gum disease is called gingivitis, and it’s basically a localized inflammatory response from your immune system.
Think of it like a small, contained campfire. It’s noticeable and definitely requires attention, but with the right actions, you can easily put it out before it spreads and causes real damage.
This is the point where the battle is entirely winnable without any lasting casualties. The infection is only in the gum tissue itself and hasn't started attacking the underlying bone that supports your teeth. It’s your body’s way of tapping you on the shoulder and saying, "Hey, we've got a problem here!"
Spotting The Early Signs of Trouble
Gingivitis is sneaky. It often whispers before it shouts, and its symptoms can be subtle enough to ignore if you aren't paying attention. But knowing what to look for means you can take action quickly and stop it in its tracks.
Keep a close eye out for these common indicators:
- Red, Swollen, or Puffy Gums: Healthy gums are firm, pale pink, and fit snugly around your teeth. Inflamed gums often look angry—redder, shinier, and more swollen than usual.
- Bleeding When You Brush or Floss: Seeing pink in the sink when you spit isn't normal. This is one of the earliest and most common signs that your gums are irritated by plaque.
- Persistent Bad Breath: While a cup of coffee or a garlicky meal can cause temporary bad breath, a constant foul taste or smell that brushing doesn't fix could be from the bacteria causing gingivitis.
- Tender or Sensitive Gums: Your gums might feel sore to the touch, especially when you're brushing or flossing.
These symptoms are your cue to step up your dental care. Ignoring them is like letting that campfire smolder, giving it the perfect chance to grow into a much larger, more destructive fire.
The most important thing to know about gingivitis is that it is 100% reversible. At this stage, no permanent damage has been done to the bone or connective tissues holding your teeth in place. It's a critical window of opportunity you don't want to miss.
How to Extinguish the Inflammation
Thankfully, reversing gingivitis doesn’t involve complex or painful procedures. It simply demands a return to the fundamentals of excellent oral hygiene. When you diligently remove the plaque causing all the irritation, you give your gums the space they need to heal and get back to normal.
Your action plan is pretty straightforward:
- Brush Thoroughly Twice a Day: Pay special attention to cleaning right along the gumline, which is where plaque loves to accumulate.
- Floss Daily (and Do It Right): Flossing is non-negotiable. It clears out the plaque and food debris your toothbrush just can't reach between your teeth and under the gums.
- Schedule Regular Professional Cleanings: Your dental hygienist has the tools to remove any plaque that has hardened into tartar, which you can’t get rid of on your own.
With just a little consistent care, you'll see the inflammation go down, the bleeding stop, and your gums become firm and healthy again. For more detailed guidance, you can learn how to reverse gingivitis at home with our dedicated guide.
Taking these simple steps slams the door shut on gingivitis and prevents it from ever advancing to a more serious stage.
When Gum Disease Becomes A Serious Threat

If gingivitis is a small, containable campfire—a clear warning sign—then periodontitis is the out-of-control wildfire that can follow. When that initial inflammation gets ignored, the infection doesn't politely stay on the surface. It digs deeper, transforming from a minor annoyance into a genuinely destructive disease.
This is the advanced stage where the real damage starts. The bacterial infection burrows below the gumline, forcing the gums to pull away from the teeth. This separation creates small, destructive spaces known as periodontal pockets. Think of them as tiny, toxic trenches around your teeth.
These pockets become the perfect breeding ground for even more aggressive bacteria, making it impossible for you to clean them out with just a toothbrush and floss. The infection is now sheltered and can thrive, leading to a vicious cycle of deeper pockets and a more severe infection. It's a problem that has been steadily growing. Data shows that from 1990 to 2021, the incidence of periodontal disease surged by over 76%, impacting nearly 90 million people worldwide. You can explore more about this alarming global increase in periodontal disease cases and its connection to changing demographics.
The Foundation Starts to Crumble
The most dangerous part of periodontitis is what happens beneath the surface, where you can't see it. Tucked away in those deep pockets, the bacteria and your body's own chronic inflammatory response begin to destroy the very structures holding your teeth in place.
It's a lot like erosion slowly wearing away the foundation of a house. The infection starts eating away at the connective tissues and, most critically, the jawbone that anchors your teeth. This destruction is slow and often painless in its early stages, but it is absolutely relentless.
As more bone and tissue disappear, you'll start to notice more severe symptoms that signal the disease has taken a firm hold.
- Receding Gums: Your teeth might start to look longer than they used to. This is because the gum tissue has pulled back, exposing more of the tooth's surface.
- Persistent Bad Breath: A foul taste or odor that just won't go away, even right after brushing, is a common sign of a deep-seated infection.
- Loose or Shifting Teeth: As the supporting bone vanishes, teeth can become wobbly. You might even notice new gaps forming between them.
- Pain When Chewing: Simple pressure on these compromised teeth can become uncomfortable or even painful.
The critical takeaway here is that the damage caused by periodontitis is irreversible. Unlike gingivitis, you cannot fix this at home. The bone that has been lost will not grow back on its own.
This is the point where professional help isn't just a good idea—it's essential. The goal is to stop the destructive process in its tracks, manage the infection, and prevent any more bone loss to save your teeth. The treatments required go far beyond a standard cleaning and involve specialized care to get deep below the gumline. You can learn more about how dentists treat this advanced stage in our guide explaining what is periodontal therapy.
Hidden Risk Factors That Fuel Gum Disease

While bacterial plaque is the spark that ignites gum disease, certain conditions and lifestyle choices act like gasoline poured on the fire. They don't necessarily start the problem on their own, but they can dramatically accelerate its progression from mild gingivitis to severe periodontitis.
To really understand what causes gum disease, we have to look beyond just brushing and flossing. Your overall health and daily habits create the internal environment where this infection can either be kept in check or allowed to run rampant.
Smoking and Tobacco Use
If gum disease is a fire, smoking is the ultimate accelerant. It seriously cripples your body's ability to fight off infection and heal itself. The nicotine and other chemicals in tobacco products restrict blood flow to your gums, essentially starving them of the oxygen and nutrients they need to stay healthy.
What does this mean in real terms? A smoker’s gums are far less capable of repairing themselves after being irritated by plaque. An infection that might have stayed as a minor case of gingivitis in a non-smoker can quickly explode into destructive periodontitis. It's no surprise that smokers are significantly more likely to develop gum disease, and treatments are often less successful.
The Diabetes Connection
Diabetes and gum disease have a dangerous two-way relationship. When blood sugar levels aren't well-controlled, it weakens the immune system, making it much harder to fight off the bacteria causing gum infections. High blood sugar can also lead to more sugar in your saliva, which is basically a feast for harmful oral bacteria.
At the same time, a severe gum infection can make it more difficult to control blood sugar levels, creating a destructive feedback loop. Managing diabetes is a critical part of managing your risk for severe periodontitis, as the two conditions can constantly make each other worse.
Hormonal Shifts and Increased Sensitivity
Hormones play a surprisingly large role in your gum health. Big fluctuations during certain life stages can make the gums extra sensitive and much more prone to inflammation.
- Pregnancy: A spike in progesterone can lead to "pregnancy gingivitis," making gums swell, bleed, and react much more strongly to even small amounts of plaque.
- Menopause: The hormonal shifts here can cause dry mouth and bone loss. Both of these increase the risk for gum disease and tooth decay.
- Puberty: That surge in hormones can increase blood flow to the gums, causing heightened sensitivity and irritation.
While these hormonal changes are completely natural, they demand extra attention to your oral hygiene routine to prevent temporary sensitivity from turning into a long-term problem.
Other Contributing Factors
Beyond these major risks, several other elements can compromise your gum health.
Key Insight: Many common medications—including certain antidepressants, antihistamines, and blood pressure drugs—can cause dry mouth (xerostomia). Saliva is your mouth's natural defense system, washing away food and neutralizing acids. A dry mouth creates the perfect breeding ground for bacteria.
Chronic stress also takes a toll by weakening your immune system, making you more vulnerable to infections everywhere, including your gums. And of course, what you eat directly impacts your oral ecosystem; you can learn more about how diet affects your dental health in our detailed guide. Finally, genetics can predispose some people to gum disease, meaning they have to be even more diligent with their care. You can find additional articles and insights on various health topics by visiting the Salthea Blog for more health insights.
The Domino Effect of Ignoring Gum Health
Ignoring the early signs of gum disease is a bit like seeing a small crack in a dam and deciding to look the other way. For a while, nothing happens. But eventually, the pressure builds, and the consequences become far more severe—and costly—than fixing the initial problem. When left untreated, gum disease sets off a chain reaction that goes well beyond your mouth, impacting your health, your confidence, and your overall quality of life.
The most direct and devastating result is tooth loss. As the infection worsens from gingivitis to the more severe stage of periodontitis, the supporting bone and soft tissues that hold your teeth in place literally begin to dissolve. Your teeth, now anchored in a crumbling foundation, become loose. Eventually, they can fall out on their own or need to be extracted.
This isn't a rare problem; it's a massive global health crisis. Research shows that severe periodontal disease affects over 1 billion people worldwide, with a global prevalence of about 12.5% as of 2021. This advanced stage is a primary driver of widespread tooth loss, which dramatically impacts well-being across the globe. You can learn more about the global burden of periodontitis and its effects in this detailed report.
From Your Mouth to Your Body
The story doesn't end with missing teeth, though. The chronic inflammation brewing in your gums doesn’t stay put. Think of the infected gum tissue as a constant, open gateway, allowing harmful bacteria and their inflammatory byproducts to slip directly into your bloodstream.
What happens in your mouth doesn’t stay in your mouth. The bacteria and inflammation from gum disease can travel throughout your body, contributing to serious systemic health conditions.
Once these troublemakers are circulating, they can trigger or worsen problems in other parts of your body. This is precisely why your oral health is such a critical piece of your entire health puzzle.
The Systemic Health Connection
A growing mountain of evidence now links advanced gum disease to a higher risk for several major health conditions. The constant, low-grade inflammation originating in your gums can fuel inflammation elsewhere, creating a dangerous domino effect of health complications.
Some of the most well-documented connections include:
- Heart Disease: The same bacteria found festering in periodontal pockets have been discovered in the fatty plaques that clog arteries, which can increase the risk of heart attack and stroke.
- Respiratory Infections: Breathing in bacteria from infected gums over long periods can lead to respiratory issues like pneumonia, particularly in older adults or those with weakened immune systems.
- Diabetes Complications: This relationship is a two-way street. Gum disease can make it harder for the body to control blood sugar, and in turn, uncontrolled diabetes creates an environment where gum disease can thrive.
- Adverse Pregnancy Outcomes: Studies have linked severe gum disease to an increased risk of premature birth and low birth weight babies.
Understanding these far-reaching consequences truly highlights the importance of being proactive. This is about so much more than just saving your teeth—it’s about protecting your overall well-being. Investing in routine check-ups is one of the most powerful steps you can take, and you can explore more about the benefits of preventive dental care right here on our site.
Common Questions About Gum Disease
Navigating the world of oral health can bring up a lot of questions. When it comes to something as common as gum disease, getting clear, straightforward answers is the first step toward taking control. Let's tackle some of the most frequent concerns people have about this condition.
Can Gum Disease Be Cured Completely?
This is one of the most important questions we hear, and the answer really depends on the stage. The fantastic news is that gingivitis, the earliest form of gum disease, is 100% curable. With a dedicated return to excellent oral hygiene—we're talking thorough brushing and daily flossing—and a professional cleaning, you can completely reverse the inflammation and get your gums back to full health.
However, the story changes once the condition advances to periodontitis. At this stage, the infection has caused irreversible damage to the bone and soft tissues that hold your teeth in place.
Key Takeaway: Periodontitis can't be "cured" in the traditional sense, because the bone that has been lost won't just grow back on its own. Instead, professional treatment focuses on stopping the disease in its tracks, managing the infection, and preventing any more damage to save your teeth.
How Quickly Does Gum Disease Develop?
There’s no single timeline for how gum disease develops; it's a highly individual process. The speed of its progression is a mix of your oral hygiene habits, your genetics, and other personal risk factors.
A mild case of gingivitis can pop up surprisingly fast. You might notice redness and bleeding gums in just a few weeks if you've been slacking on your brushing and flossing.
Developing advanced periodontitis, on the other hand, is usually a much slower burn that can take years. The rate it advances is heavily influenced by factors like:
- Smoking: Tobacco use can put the disease on the fast track.
- Systemic Health: Conditions like unmanaged diabetes can speed up bone loss significantly.
- Genetic Susceptibility: Some people are simply more prone to developing serious gum disease.
- Oral Hygiene: A diligent routine is your best defense and can hold the disease at bay for a long, long time.
Someone with great hygiene and well-managed risks might never see their gingivitis progress. On the flip side, a person with poor habits and multiple risk factors could see a much faster decline.
Is Gum Disease Contagious?
This is a very common worry, especially for people thinking about their partners or family. The bacteria that cause gum disease can be transferred through saliva—by sharing drinks, utensils, or kissing. However, this doesn't mean the disease itself is contagious.
Think of it this way: just being exposed to the bacteria isn't enough to get the disease. Whether gum disease develops depends almost entirely on how those bacteria interact with your body’s unique environment.
Your personal oral hygiene, the strength of your immune system, and your genetic makeup are the real deciding factors. For a deeper dive into common concerns like this one, you might find our comprehensive periodontal therapy FAQ helpful. In short, you can’t "catch" gum disease like you would a cold.
At Beyond Dental Care, we believe that clear information is the foundation of great oral health. If you have more questions or are concerned about the health of your gums, our team in Glendale, Arizona, is here to provide the expert, patient-focused care you deserve. Schedule a consultation with us today to take the first step toward a healthier smile.
